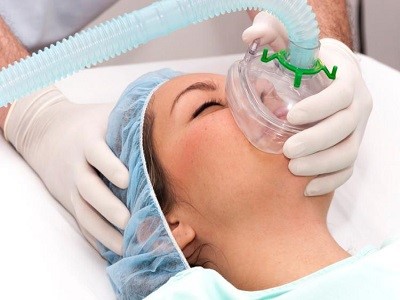
Rhinoplasty (RIE-no-plas-tee) is surgery that changes the shape of the nose. The motivation for rhinoplasty may be to change the appearance of the nose, improve breathing, or both.
The upper portion of the structure of the nose is bone, and the lower portion is cartilage. Rhinoplasty can change bone, cartilage, skin, or all three. Talk with your surgeon about whether rhinoplasty is appropriate for you and what it can achieve.
When planning rhinoplasty, your surgeon will consider your other facial features, the skin on your nose, and what you would like to change. If you’re a candidate for surgery, your surgeon will develop a customized plan for you.
Sometimes part or all of a rhinoplasty is covered by insurance.
Why it’s done
Rhinoplasty can change the size, shape, or proportions of your nose. It may be done to repair deformities from an injury, correct a birth defect or improve some breathing difficulties.
Risks
As with any major surgery, rhinoplasty carries risks such as:
- Bleeding
- Infection
- An adverse reaction to the anesthesia
Other possible risks specific to rhinoplasty include but are not limited to:
- Difficulty breathing through your nose
- Permanent numbness in and around your nose
- The possibility of an uneven-looking nose
- Pain, discoloration, or swelling that may persist
- Scarring
- A hole in the septum (septal perforation)
- A need for additional surgery
Talk to your doctor about how these risks apply to you.
How you prepare
Before scheduling rhinoplasty, you must meet with your surgeon to discuss important factors that determine whether the surgery is likely to work well for you. This meeting generally includes:
- Your medical history
The most important question your doctor will ask you is about your motivation for surgery and your goals. Your doctor will also ask questions about your medical history — including a history of nasal obstruction, surgeries, and any medications you take. If you have a bleeding disorder, such as hemophilia, you may not be a candidate for rhinoplasty.
- A physical exam
Your doctor will conduct a complete physical examination, including any laboratory tests, such as blood tests. He or she also will examine your facial features and the inside and outside of your nose.
The physical exam helps your doctor determine what changes need to be made and how your physical features, such as the thickness of your skin or the strength of the cartilage at the end of your nose, may affect your results. The physical exam is also critical for determining the impact of rhinoplasty on your breathing.
- Photographs
Someone from your doctor’s office will take photographs of your nose from different angles. Your surgeon may use computer software to manipulate the photos to show you what kinds of results are possible. Your doctor will use these photos for before-and-after assessments, reference during surgery, and long-term reviews. Most importantly, the photos permit a specific discussion about the goals of the surgery.
- A discussion of your expectations
You and your doctor should talk about your motivations and expectations. He or she will explain what rhinoplasty can and can’t do for you and what your results might be. It’s normal to feel a little self-conscious discussing your appearance, but you must be open with your surgeon about your desires and goals for surgery.
If you have a small chin, your surgeon may speak with you about performing a surgery to augment your chin. This is because a small chin will create the illusion of a larger nose. It’s not required to have chin surgery in those circumstances, but it may better balance the facial profile.
Once the surgery is scheduled, you’ll need to arrange for someone to drive you home if you’re having an outpatient surgery.
For the first few days after anesthesia, you may have memory lapses, slowed reaction time, and impaired judgment. To arrange for a family member or friend to stay with you a night or two to help with personal care tasks as you recover from surgery.
- Food and medications
Avoid medications containing aspirin or ibuprofen (Advil, Motrin IB, others) for two weeks before and after surgery. These medications may increase bleeding. Take only those medications approved or prescribed by your surgeon. Also, avoid herbal remedies and over-the-counter supplements.
If you smoke, stop smoking. Smoking slows the healing process after surgery and may make you more likely to get an infection.
What you can expect
Rhinoplasty does not have an ordered series of steps. Each surgery is unique and customized for the specific anatomy and goals of the person having the surgery.
During the surgery
Rhinoplasty requires local anesthesia with sedation or general anesthesia, depending on how complex your surgery is and what your surgeon prefers. Discuss with your doctor before surgery which type of anesthesia is most appropriate for you.
- Local anesthesia with sedation
This type of anesthesia is usually used in an outpatient setting. It’s limited to a specific area of your body. Your doctor injects a pain-numbing medication into your nasal tissues and sedates you with medication injected through an intravenous (IV) line. This makes you groggy but not fully asleep.
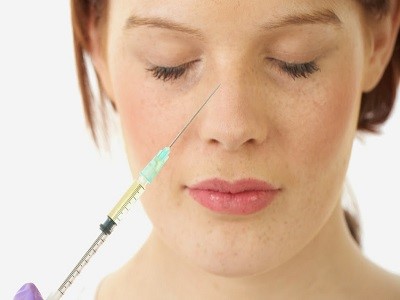
- General anesthesia
You receive the drug (anesthetic) by inhaling it or through a small tube (IV line) placed in a vein in your hand, neck, or chest. General anesthesia affects your entire body and causes you to be unconscious during surgery. General anesthesia requires a breathing tube.
Rhinoplasty may be done inside your nose or through a small external cut (incision) at the base of your nose, between your nostrils. Your surgeon will likely readjust the bone and cartilage underneath your skin.
Your surgeon can change the shape of your nasal bones or cartilage in several ways, depending on how much needs to be removed or added, your nose’s structure, and available materials. For small changes, the surgeon may use cartilage taken from deeper inside your nose or your ear. For larger changes, the surgeon can use cartilage from your rib, implants, or bone from other parts of your body. After these changes are made, the surgeon places the nose’s skin and tissue back and stitches the incisions in your nose.
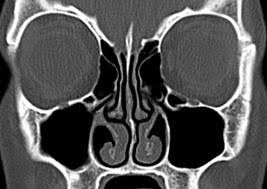
If the wall between the two sides of the nose (septum) is bent or crooked (deviated), the surgeon can also correct it to improve breathing.
After the surgery, you’ll be in a recovery room, where the staff monitors your return to wakefulness. You might leave later that day or, if you have other health issues, you might stay overnight.
After the surgery
After the surgery, you need to rest in bed with your head raised higher than your chest, to reduce bleeding and swelling. Your nose may be congested because of swelling or from the splints placed inside your nose during surgery.
In most cases, the internal dressings remain in place for one to seven days after surgery. Your doctor also tapes a splint to your nose for protection and support. It’s usually in place for about one week.
Slight bleeding and drainage of mucus and old blood are common for a few days after the surgery or after removing the dressing. Your doctor may place a “drip pad” — a small piece of gauze held in place with tape — under your nose to absorb drainage. Change the gauze as directed by your doctor. Don’t place the drip pad tight against your nose.
To further lower the chances of bleeding and swelling, your doctor may ask that you follow precautions for several weeks after surgery. Your doctor may ask you to:
- Avoid strenuous activities such as aerobics and jogging.
- Take baths instead of showers while you have bandages on your nose.
- Not blow your nose.
- Eat high-fiber foods, such as fruits and vegetables, to avoid constipation. Constipation can cause you to strain, putting pressure on the surgery site.
- Avoid extreme facial expressions, such as smiling or laughing.
- Brush your teeth gently to limit movement of your upper lip.
- Wear clothes that fasten in the front. Don’t pull clothing, such as shirts or sweaters, over your head.
In addition, don’t rest eyeglasses or sunglasses on your nose for at least four weeks after the surgery, to prevent pressure on your nose. You can use cheek rests, or tape the glasses to your forehead until your nose has healed.
Use SPF thirty sunscreen when you’re outside, especially on your nose. Too much sun may cause permanent irregular discoloration in your nose’s skin.
Some temporary swelling or black-and-blue discoloration of your eyelids can occur for two to three weeks after nasal surgery. Swelling of the nose takes longer to resolve. Limiting your dietary sodium will help the swelling go away faster. Don’t put anything such as ice or cold packs on your nose after surgery.
Your nose changes throughout your life whether you have surgery or not. For this reason, it’s difficult to say when you have obtained your “final result.” However, most of the swelling is gone within a year.
Results
Very slight changes to the structure of your nose — often measured in millimeters — can make a large difference in how your nose looks. Most of the time, an experienced surgeon can get results both of you are satisfied with. But in some cases, the slight changes aren’t enough, and you and your surgeon might decide to do a second surgery for further changes. If this is the case, you must wait at least a year for the follow-up surgery, because your nose can go through changes during this time.
Tips that are necessary after discharge from the hospital and returning home:
- Avoid eating hard foods that require prolonged chewing (such as sandwiches, steaks, and kebabs) and foods that you know you are allergic to.
- Fruits, fish, shrimp, and omega-three are highly recommended
- Limit salt intake in your diet for a while.
- Avoid intense exercise activities such as weightlifting for about a month.
- Do not expose to stove, heat, and strong sunlight for the first few weeks.
- Avoid lifting heavy objects and bending.
- For up to 48 hours, apply a cold compress to the face and graft site (if present), then a warm compress will accelerate the absorption of bruises and swelling. The pain peaks for up to three days and then subside, during which time painkillers are recommended.
- During the few weeks after the operation, breathing becomes difficult due to the accumulation of secretions inside the nose, so you can use the saline solution (washing serum) several times a day. Using a 20 cc needleless syringe, remove the serum and pour it into the nose, allowing the discharge to be flushed out.
- Avoid smoking and other tobacco.
- Do not force-squeeze nasal discharge for two weeks after surgery.
- Usually, glue the nose for 3 to 4 months according to the doctor’s instructions.
- Be careful not to get any hit to your nose, for example, sleep in an open arch and use clothes with buttons and zippers.
- Sneeze with your mouth open and avoid intense facial movements while laughing and crying.
- Swimming, diving, sunbathing, sauna are prohibited for 1 to 2 months.
- To reduce facial swelling, keep your head higher than usual when resting
- Avoid wearing sunglasses and glasses for a month. If necessary, attach the glasses to the forehead with anti-allergy glue.
- It is necessary to observe personal hygiene and stay away from cold environments and people with colds.
- Take medications prescribed by your doctor (such as antibiotics at regular hours) as directed.
- Follow up with your doctor after the operation and get the necessary checkups.
Visiting doctor by this reasons
- Bleeding or swallowing blood and shortness of breath and dizziness.
- If a severe hit to the nose has caused significant bleeding or swelling.