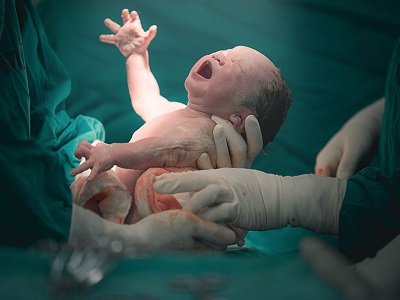
Understanding the stages of natural childbirth is the basis of preparing for the birth of a healthy baby. It is better for women to spend time during their pregnancy and get acquainted with the turning points of natural childbirth. But keep in mind that the signs and symptoms of natural childbirth are not the same for all women.
Childbirth begins with labor pains. The uterus is made up of strong muscle tissue that relaxes during pregnancy due to hormonal changes. But with the onset of labor, progressive contractions occur. Uterine contractions provide enough force for the fetus to exit as well as dilate the cervix. Gradually, following labor pains, the cervix opens and labor continues.
If there is a disorder in any of these stages, the delivery process will not progress and the health of the mother and fetus may be endangered.
About 85% of deliveries do not require any treatment process and are performed naturally. Only less than 15% of them need a cesarean section. Of course, it is worth noting that this diagnosis is possible in most cases with the onset of labor, and early detection of whether or not a woman can have a normal delivery is almost impossible.
Symptoms of the onset of normal labor
Become light
Becoming light is a term used when the time of delivery approaches when the fetal head is lowered towards the pelvis. Lightening may occur two weeks before delivery, or it may not occur at all. There is a lot of pressure on the mother’s bladder before she experiences Lightening during pregnancy, which is more when urinating.
Many women breathe easier after this stage because the pressure on the diaphragm decreases.
Plug mucus discharge (colored or brown discharge)
Plug mucus can be another sign of the time of delivery. Plug mucus is caused by the cervical glands, which normally block the entrance to the cervix and prevent infection. plug Mucous are colored or brown discharge. This mucus comes out of the cervical glands with a small amount of blood when the fetal head is placed on the cervix. plug mucous discharge may occur days before or even after the onset of labor. Plug mucus secretion is common after the vaginal examination.
Water bag rupture
Spontaneous rupture of the fetal membrane is called “rupture of the amniotic sac.”
The fetal membrane is the membrane that surrounds the baby, and when it ruptures, clear amniotic fluid comes out of the vagina.
Rupture of membranes usually does not occur until labor begins.
Intermittent contractions
Natural childbirth begins with the onset of contractions. At this stage, the cervix becomes thinner.
Types of intermittent contractions during natural childbirth include:
Irregular contractions. Known as “false normal births”, they occur in the third trimester and last until the end of pregnancy. Irregular contractions are not necessarily a sign of impending labor. Some women experience these contractions even in the second trimester of pregnancy. They are usually milder than normal labor contractions and do not occur at regular intervals.
Natural childbirth consists of three stages
The first stage is from the onset of contractions or actual pain to the complete opening of the cervix. This stage lasts about 6 to 20 hours in the first delivery and 3 to 14 hours in subsequent deliveries.
Hospitalization
In a normal delivery, hospitalization usually occurs when the cervix is at least 4 cm open, so when visiting the hospital after an internal examination by a doctor or midwife, it may be in one of the following situations:
- The cervix has not yet opened 4 cm, in which case the doctor or midwife may allow you to return home or walk to the hospital, ensuring that your condition and that of the fetus are well by controlling the vital signs and hearing the sound of the fetus’s heart. If you return home, remember to go to the hospital immediately if the pain gets worse or if you bleed or water discharge. It is better to avoid eating solid and enormous foods at this time.
- The cervix is open by 4 cm or more. In this case, you will be admitted and at the time of admission, the following will be done for you:
- Filing and be admitted to a pain or delivery room
- Change clothes and wear maternity clothes
- Take a history and control vital signs
- Perform the required tests
- Examine the sound of the fetal heart and control the movements of the fetus
- Internal examination (vaginal)
- Taking blood vessels and injecting serum if needed
- Prohibition of eating and drinking
After being admitted to a pain room or maternity ward at regular intervals, vital signs (blood pressure, pulse, respiration, and temperature) are measured and the fetal heart rate is monitored.
An internal examination is also done to check the progress of the birth. It is recommended to empty your bladder every 2 hours.
At the time of admission to a normal delivery room in the pain room, you can be in any of the following positions to feel more comfortable:
Four-knee position with the body pulled forward.
- When standing, place one foot on a step or height.
- Lying on your side, bend the upper leg from the knee and place it on the lower leg (it is better to place a pillow between the two legs).
- In the position of four legs and in a position where you transfer the weight of your body to the hips.
Gradually, as the cervix opens and softens, the fetal head descends into the birth canal and moves toward the vaginal opening. The fetus enters the birth canal naturally. At this point, you should be in a position where less pressure is applied to the last vertebrae of the waist. Therefore, postures such as lying on your side, prostrating on all fours, and squatting are recommended, and consistent changes in posture can reduce fatigue, improve blood circulation, and improve labor. Note that before the fetus enters the pelvis, the mother tends to be more upright or walk, but when the fetus enters the pelvis, standing and walking become difficult for the mother and can be in other positions.
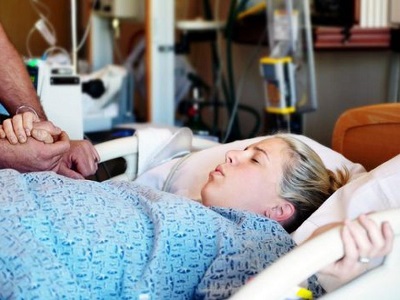
The second stage involves the complete dilation of the cervix until the baby is born. The average time for this step is about 50 minutes.
Once the cervix is fully open, the second stage of labor begins when you are asked to sit on a crib in a semi-sitting position and place your feet on a special pedal (this position is typically used in a hospital for normal delivery. This condition usually helps the fetus’s head, shoulders, and body to come out. If you need to make changes or be in a special position during labor, the delivery manager will guide you. At this point, the fetal heart rate will also be monitored.
As the fetal head descends and approaches the exit of the birth canal, you may feel pressure or expulsion. Uterine contractions, along with controlled squeezing, cause the fetus to leave the birth canal (vagina). This canal has a good curvature and the body of the fetus naturally adapts to its shape when it comes out. At this stage, it is necessary to actively participate in your delivery and cooperate with the delivery manager. Using breathing skills and relaxing your muscles will help you reduce the time it takes to give birth. The most important maneuver you can do is to bend and bring your knees together towards the chest with the help and guidance of the delivery manager, while the head is completely on the bed, and with the onset of contraction, inhale deeply and exhale. Empty yourself as you contract your abdominal muscles to push the fetus out.
At the end of this stage, the midwife will remove your baby while pushing you.
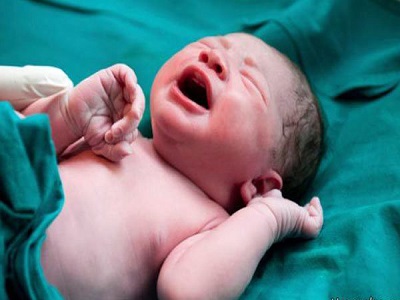
The third stage begins after the baby is completely removed. The third stage of labor begins.
The first step in this step, after cleaning the baby’s mouth and nose, is to cut the umbilical cord. It takes time for the placenta to come out and it is usually accompanied by bleeding. The time required for placental abruption is 5 to 30 minutes after the fetus leaves. During this time, the delivery agent takes care of the baby and prepares him for breastfeeding. With the complete removal of the placenta and embryonic membranes, the third stage of labor ends, and at the end of this stage, the delivery manager examines the birth canal for the presence of a rupture.
In some women, a small incision is made in the midway area at the end of the second stage of labor to make it easier for the fetal head to come out after the local anesthetic is injected. This incision is sutured in several layers after the placenta is removed. The number of sutures varies according to the location and size of the incision, the suture is absorbable and does not need to be pulled. The genital area is then washed and the mother is prepared to be transferred to the postpartum room. The best thing to do after giving birth is to gently hug your baby and let him or her enjoy the blessings of the colostrum by sucking on the breast.
A few recommendations for patients companion
Immediately after delivery (the first few hours) the companion plays a very important role. you can:
If you have a clot or excessive menstrual bleeding (so that blood collects under the mother’s buttocks), tell the delivery manager about dizziness, loss of consciousness, and shortness of breath immediately. It is very important to pay attention to these symptoms and take timely action to maintain the mother’s health.
Assist the mother in breastfeeding immediately after delivery.
Encourage the mother to empty her bladder in the early hours after giving birth.
- Help the mother to slowly get out of bed and walk for a few hours after giving birth.
Sudden arousal after childbirth, especially for the first time, causes a drop in blood pressure and the mother loses consciousness.
Pain control during labor
There are several different painkillers to control pain. But many women refuse to take medication to control pain during childbirth, while others choose medical methods to control pain. Local anesthesia is another option to control pain during labor. Research has shown that local anesthetics are more effective than injectable medicines in controlling pain. Women who decide not to take pain killer can use breathing techniques to control the pain. Meditation and yoga techniques have also been helpful.
Monitoring during childbirth
The type of monitoring chosen depends on different factors and will be different in different women. In the first stage of labor, pelvic exams are performed to check for opening and thinning of the cervix. The baby’s heart rate is usually checked intermittently with the device, or continuous electronic monitoring of the fetus may be performed. External monitoring of the fetus is done by placing a transducer on the wall of the mother’s abdomen. The transducer detects the fetal heartbeat and displays it on a monitor. Internal monitoring is another method used to monitor the fetal heart rate. Using this technology, a small receptor passes through the cervix and attaches to the scalp of the fetus.
Postpartum care
After delivery, the health of the baby is usually the main priority of the parents. But postpartum care is important for the mother’s health. Pregnancy changes a woman’s body, and these changes continue at birth.
Some postpartum changes include:
Vaginal pain
If the mother has an episiotomy or ruptured vagina during childbirth, the wound may take several weeks to heal. Deeper wounds take longer to heal.
Women should consider the following strategies for vaginal pain:
- Sit on an empty pillow or ring.
Cool the wound with an ice pack or place a cold tissue between the sanitary pads at the wound.
- Eat an over-the-counter painkiller. If necessary, consult your doctor about an anesthetic spray or cream.
To prevent constipation, talk to your doctor about using a stool softener or laxative.
Severe or persistent pain can be a sign of infection, in which case see your doctor.
Vaginal discharge
Mothers may have vaginal discharge consisting of mucus and blood (spots) for weeks after delivery. The discharge will be red for the first few days, then decrease and become watery and change to pink, white or yellow. See your doctor if you have severe vaginal bleeding, especially if it is accompanied by pelvic pain, fever, or uterine allergy.
Contractions
Women may experience temporary contractions during the first few days after giving birth. These contractions, which are often similar to menstrual contractions, help prevent excessive bleeding by squeezing blood vessels in the uterus. Swelling of the legs during breastfeeding is common due to the release of a hormone called oxytocin. In these cases, your doctor may recommend a painkiller.
urinary incontinence
Pregnancy, cesarean section, and natural childbirth can weaken or injure the pelvic floor muscles.
Weakening of the pelvic floor muscles in women causes a few drops of urine to leak when sneezing, laughing, or coughing (stress incontinence). These problems will usually improve within a few weeks. But in some cases, it may continue in the long run. In these cases, it is better for pregnant women to use a sanitary pad and do Kegel exercises. To do proper Kegel exercises, women can relax the muscles of the chest, abdomen, thighs, and buttocks. Squeeze the pelvic floor muscles and hold them in place for 5 to 10 seconds. Simultaneously squeeze the anus and pull your vagina up quickly, immediately tightening and releasing the muscles. Loosen them for 5 to 10 seconds and repeat.
It is best to do these exercises at least three times a day, 10 to 15 times in a row.
Hemorrhoids and defecation
Pain and swelling near the anus at the same time as defecation can be symptoms of hemorrhoids. Women can use hemorrhoid cream after childbirth to cure hemorrhoids and relieve discomfort. Soak your anal area in warm water for two to three times a day for 10 to 15 minutes. To soften and dilute stools, eat high-fiber foods, including fruits, vegetables, and whole grains, and drink plenty of water. See a doctor if necessary.
Breast tenderness
A few days after birth, a woman’s breasts may become firm, soft, and tender. Frequent breastfeeding is recommended to prevent or minimize breast tenderness. If the breast, including dark areas of skin around the nipple, is tender, the baby may have difficulty breastfeeding. To help the baby suckle, it is best to use the hand to pump the breast. Mothers should follow the tips related to breastfeeding and increasing breast milk.
Hair loss and skin change
During pregnancy, increased hormone levels increase hair loss. Women will experience hair loss for up to five months after giving birth. The symptoms of stretch marks do not disappear after childbirth, but eventually, fade over time. In addition, dark patches on the face (cloasma) gradually disappear.
Mood swings
Childbirth causes mood swings. Many mothers experience a period of anxiety or depression that is sometimes referred to as a postpartum depression. Postpartum depression usually goes away in two weeks. Women should take care of themselves during this period. Express your feelings, and ask for help from your partner, family, or friends. If after a while the symptoms do not improve and the woman has difficulty caring for the child or doing daily chores or has thoughts of harming herself or the child, she should see a counselor or psychologist.
Symptoms of postpartum depression include:
- Anxiety
- Sorrow
- Excessive fatigue
- Sleep disorder
- Loss of appetite
- Severe mood swings
Weight Loss
Most women lose 6 kg during childbirth. The cause of this weight loss is the discharge of the baby, placenta and amniotic fluid. Then, a healthy diet and regular exercise will help the woman reach her previous weight.
Postpartum examination and examination
It is recommended that the mother see her doctor in the first 3 weeks after delivery. During this visit, the doctor will check your mental and physical condition and advise you on how to prevent the next pregnancy and the distance between deliveries. Provides information on baby care and nutrition, sleep habits and issues related to the patient’s fatigue, and performs a physical examination. Physical examination includes examination of the abdomen, vagina, cervix, and uterus to ensure the mother is fully recovered.
If you are hospitalized, follow these tips:
- Fast until delivery. Or at least avoid heavy foods such as milk, liver and eggs.
- If you have makeup and nail polish, remove it.
- Hair at the operation site needs to be shaved before delivery.
- Empty the bladder (urine) before transferring to the delivery room.
- When entering the maternity ward, remove jewelry, metal objects, head clips, dentures, etc.
- Take off all clothes (underwear, socks, etc.) and wear maternity clothes.
- If you have a history of illness, report the history of allergies (medication, food) to the nurse and physician.
- Tell your doctor and nurse if you have a specific illness that you are being treated for, as your medication may need to be discontinued and replaced with new medications.
- If you come in preparation for delivery (non-emergency), use laxatives so that complete defecation is done before delivery so that you have a comfortable and clean delivery.
- Avoid foods that cause constipation, diarrhea, vomiting and bloating after childbirth.
- To get out of bed, first sit on the edge of the bed for a while and hang your legs, if you do not feel dizzy, blurred vision and… walk with the help of the care team.
- Get out of bed and walk several times an hour for mobility and activity.
- There may be significant bleeding up to 24 hours after delivery and the blood volume may gradually decrease but vaginal discharge may be seen for up to a month.
- Report dizziness, loss of consciousness, shortness of breath immediately if there is a clot or excessive menstrual bleeding (so that blood has collected under the mother).
- Empty your bladder to prevent bleeding in the early hours after delivery.
- To prevent urinary tract infections and genital infections, wash and dry the front and back with soap and baby shampoo or shampoo after each defecation and urination.
- Report pain or discomfort to the nurse before leaving the bed.
- Drink plenty of fluids, even water, to replenish lost fluids and increase milk supply.
- To prevent deep vein thrombosis, gradually get out of bed and walk for a few hours after delivery.
- Wash your hands with soap and water before each feeding and use only plain water to clean your nipples.
- Frequent breastfeeding causes the uterus to shrink and bleeding to decrease.
- If prescribed by a doctor, painkillers and vitamins are prescribed by the nurse at a specific time.
Follow the tips that are necessary after discharge from the hospital and return home.
- Avoid bloated and slow-digesting foods and eat high-fiber diets (fruits and vegetables) and fluids to prevent constipation.
- Avoid pushing, lifting heavy objects and driving (as long as your doctor advises).
- It is better to refrain from sexual intercourse for 4 weeks after delivery with the advice of a doctor.
- Take a shower on the second day after delivery.
- Wash your hands with soap and water before each feeding and use only plain water to clean your nipples.
- In the first two or three days after delivery, the amount of milk secretion is low, which gradually increases as the baby sucks.
- Avoid sitting in a chair for long periods of time and putting pressure on your knees, putting your feet on top of each other, and being immobile.
- Observe personal and genital hygiene. Wash the genital area from front to back, and after each urination and defecation, if you have stitches, wash that area with lukewarm water and dry it with a clean, disposable towel.
- With your doctor’s permission, you can start exercising in the first weeks after giving birth. Because you are breastfeeding your baby, you can not go on a weight loss diet, but you can get the energy you need to feed your baby by reducing your intake of fats, sweets, and substituting fruits, vegetables, and protein in your daily diet.
- Change underwear daily and use cotton underwear and avoid wearing clothes containing synthetic fibers and tights and plastic socks.
- Underwear should always be dry and avoid getting wet.
- If you are prescribed medicine, take it at regular intervals and for a full period according to your doctor’s instructions.
- Take painkillers as prescribed by your doctor.
- Visit a nearby health center for postpartum care, baby care, and vaccinations.
- See your doctor 7-10 days after delivery. Breastfeed your baby regularly.
- Regular breastfeeding is effective in establishing an emotional bond between mother and baby. It also reduces postpartum hemorrhage.
- Have enough rest between daily activities. Breastfeed from both breasts and wash the nipples with lukewarm water before and after breastfeeding.
See the hospital or doctor if you see the following
- In case of redness or purulent discharge from the incision
- In case of heavy bleeding or bad discharge, fever and chills, paleness, leg pain, dizziness, shock symptoms (weakness, coldness of the limbs, rapid breathing, dizziness and headache), impaired urination and defecation
- If bleeding increases to the point that more than one sanitary pad is wet every hour.
- Continued heavy, bright red bleeding after the first week
- Re-change the color of the bleeding to bright red
- In case of chest tightness, pain, redness and inflammation of the chest
- Rinse the sutures with serum.
- Avoid sexual intercourse for 4-6 weeks.
- Wash the stitches with soap scum. Take a bath once a day. Change underwear and sanitary pads at short intervals.
- Other concerns or emergencies